Part 1 of 2

Preamble
On February 3rd, 2015, members of the UK’s parliament voted in favour of draft for regulations in mitochondrial donation (UK Parliament, 2015). This draft is first of its kind. It is altering the egg itself. The popular name for this new form of IVF is, three-parent baby (“Foetus with three parents created,” 2003). There has been much debate about it amongst the public (Robin Clarke and Remco van der Stoep, 2013) and that was reflected in parliament. Mitochondrial replacement therapy (MRT) is the proper name given to the process that leads to fertilising an egg made of nuclear DNA from one woman and mitochondrial DNA from another woman. The UK’s Human Fertilisation Laws were amended to accommodate this new therapy (UK Legislation, 2008). The regulations on Mitochondrial Donation will come into effect from 29th October 2015 (Human Fertilisation and Embryology (Mitochondrial Donation) Regulations 2015, 2015). The conception of a baby using genetic material from three parties could be as soon as in the year 2016. The potential effects are vast, varied and unknown. The issues surrounding this technique range from both an intellectual ethical view as well as its practical implementable form.
Jane Ellison, the Parliament’s Under Secretary for Health came under heavy scrutiny by other Members of Parliament. There were concerns for the safety of the technique itself, the possibility of nuclear DNA alteration, germ-line modification as a form of genetic modification, allegations of breaking European Union laws on clinical trials, status of mitochondrial donor as a parent, FDA’s disapproval, the deliberate destruction of embryo, lack of clinical trials, prevention rather than cure, risk to females born and rushing into this decision (Human Fertilisation and Embryology (Mitochondrial Donation) Regulations 2015, 2015).
This article aims to explore the technique behind mitochondrial donation, why it could be needed and then the ethical issues surrounding it. In order to appreciate fully the heated debate put up in the UK parliament, I will explore what other countries have done in the past. There will be a discussion of findings from various scholars in the Muslim region and their opinions on this vastly bubbling topic.
Explanation of the technique
Prevalence and disease
In 2004, it was found that one in 8,500 in the UK carried mitochondrial defect to an amount that would cause disease (Schaefer et al., 2004). However, one in 200 carried mitochondrial DNA defect but it did not cause disease (Elliott et al., 2008). Unfortunately, mitochondrial DNA defect increases over generations. Figures have not been accurate because mitochondrial defect causes a range of diseases and severity, which can be misdiagnosed and defects can also be caused by defect in mutated mitochondrial genes in the nuclear DNA.
The diseases caused by defective mitochondria are based on the number of mutated mitochondria. A person with a high mutation load will express an equally severe spectrum of diseases as compared to one with a low mutation load. This is because healthy mitochondria will not be able to make up in function for the mutated ones (Taylor and Turnbull, 2005). Briefly, the diseases related to mitochondrial defect are, Leber’s hereditary optic neuropathy (LHON), which causes blindness, as well as fast optic nerve death in young adulthood; Leigh’s disease (NARP), which causes neuropathy, ataxia, retinitis, pigmentosa, mental retardation and lactic acidosis; MERRF (myotonic epilepsy, ragged red fibres); pyruvate dehydrogenase complex deficiency (PDCD/PHD) and MELAS (mitochondrial encephalopathy, lactic acidosis, stroke-like episodes, sensori-neural deafness)(“Types of Mitochondrial Disease - The United Mitochondrial Disease Foundation,” n.d.). In all, deterioration from mitochondrial defect is swift, painful and life-span is extremely low. A person with more than three affected organs is usually suspected to have mitochondrial defect (“Possible Symptoms,” 1996). A baby born can perhaps live up to the age of two years and maximum late teens. However, their quality of life is extremely poor.
Cause of mitochondrial disease
Mitochondrial disease is caused by mutation in the genes responsible for mitochondria. These genes are found in either the nucleus or the mitochondria itself. For the therapy of mitochondrial donation, we are only interested in mitochondrial disease caused by mutation in mitochondrial DNA.
Each cell contains between 1000-2000 mitochondria. Their function is to release energy in the form of ATP from glucose. These organelles are so well defined structurally that they are similar to the prokaryotes alpha-proteobacteria (Gray et al., 2001). Throughout respiration, different controlled biochemical processes take place that enable release of ATP. Glycolysis is the conversion of glucose to pyruvate. The Kreb’s cycle takes over in the mitochondrial matrix, following which is oxidative phosphorylation, which releases ATP.
To contextualise, mitochondria are wholly responsible for providing energy for healthy cell function. Diseases relating to the mitochondria have a pleiotropic effect and hence they are swiftly debilitating. They affect the vital organs such as the brain, heart, liver, skeletal muscles, kidney, endocrine and respiratory systems. This can lead to muscle weakness and pain, in other words, loss of motor control. There are gastro-intestinal disorders, as well as poor growth. Other diseases include those relating to the heart and liver, including diabetes. Seizures can occur too, and visual or hearing problems. There is a higher likelihood of infection along with developmental delays.
Mitochondrial disorders affect the release of ATP in the oxidative phosphorylation cycle in the mitochondria. This causes a fundamental problem in energy release thereby preventing full function of the cells involved.
Mitochondrial DNA
Mitochondria are the only organelles; apart from the nucleus, which have their own DNA (“Mitochondrial DNA,” 2013). Mitochondrial DNA is circular, unlike nuclear DNA (nDNA) which has a double helix strand and houses 20-30,000 genes. To create a mitochondrion, 3,000 genes are required. Of these 3,000 genes, 37 alone are found encoded by the mitochondrial DNA (mtDNA). The rest of the genes encoding for the mitochondria are found in the nuclear DNA. Mitochondrial defect can be result of either mutation in nuclear DNA or mtDNA. The questionable genes are the 37 genes (0.1% of the total number of genes) found solely in the mitochondrial matrix that are the centre of debate in mitochondrial donation (Rodney Shackelford, 2011). These 37 genes impact the oxidative phosphorylation process in the mitochondria. The process by which energy currency ATP is released.
In the matrix of the mitochondria lies mtDNA. This circular mtDNA has almost no ‘checking features’ in replication. This can lead to errors or mutations occurring quite easily (www.mitomap.org, 2013).
Inheritance of mitochondrial DNA
Mitochondrial DNA is inherited entirely from the mother. This is in contrast to the nuclear DNA which is a result of recombination from genetic material in the egg and sperm. The haploid mode of inheritance of the mtDNA brings about its own unique features.
Let us first compare and contrast the modes of inheritance. Firstly, when fertilisation takes place, nDNA undergoes meiosis. This is where the pronuclear containing nDNA of both egg and sperm come into close contact with one another, their chromosomes align themselves to form a spindle and the zygote is formed. Whilst this is happening, the mtDNA in the ooplasm is simply replicated onto daughter cells. Technically, it is not actively partaking in the process of fertilisation and simply providing energy for it to occur. The defective mitochondria are only passed down to the offspring through the mother. Secondly, the sperm itself loses its mitochondria in the process of fertilisation and thus only maternal mitochondria are passed on. If a man has mtDNA defect, he cannot pass it onto his offspring (Brown et al., 2006).
Although mitochondrial defect can be due to nuclear DNA encoding for the mitochondria, MRT is concerned only with those disorders caused solely by defect in the mitochondria caused by its own 37 genes.
Another interesting aspect of note is, the ‘mitochondria bottleneck’ (Wai et al., 2008). This occurs when affected mitochondria in ooplasm are replicated on to daughter cells. As these cells divide, so too the defected mitochondria. These cells then further divide along to form an embryo, the growth of which will turn into a baby. The resultant effect is an amplification in the number of affected mitochondria from mother to child. Now if this baby is a girl, she will already have eggs with mitochondrial defect. This defect will also be more so than her mother due to the ‘bottle-neck effect’. Over generations the mutation load of defected mitochondria increases to a symptomatic end that a human born cannot live to full extent.
Would it fulfil an urgent need that people could benefit from?
Currently, there is no cure for mitochondrial disease. Treatment methods offered are those of alleviating symptoms caused. They can be through prescribing anti-convulsants for their seizures, special diet, regular supplements, and little exercise. All the while the patient is asked to keep their life stress free and relax (Bruce H. Cohen, 2000). Constant nutrition is important to maintain function. The aim of all these is to avoid an energy crisis. On the other hand, a couple can undergo prenatal screening to rule out those eggs with significant mitochondrial defect. This can prove difficult in some cases because there are women whose eggs have a strong concentration of defected mitochondria. These are the women best suited for mitochondrial donation.
Another form of ‘treatment’ is the use of pre-implantation genetics (PGD) or prenatal diagnosis (PND). The aim of both techniques is to eradicate the embryo with high likelihood of mitochondrial disorder. This can be a solution for those women who are not badly affected by mitochondrial disease. However, when mitochondrial defect is such in a woman that all are eggs are highly affected, then PGD and PND are not even an option. There is no possibility in of selecting an embryo less affected in such cases.
The prevalence of mitochondrial disease caused by either nuclear or mitochondrial genes is 1 in 5000. It is thought approximately 1 in 250 live births have mtDNA defect, although most will not be symptomatic. Overall, 1 in 10,000 adults in the UK are severely affected by mitochondrial disease. MtDNA defect is considered to be the leading cause of inherited neuromuscular disorders. On the other hand, sickle cell disease, known to be the most common inherited disease affects 1 in 2000 babies born. This shows the number of people that can potentially be cured of mitochondrial defect through the novel techniques proposed in mitochondrial donation.
The Proposed Techniques for Mitochondrial Replacement Therapy (MRT)
The UK laws have been altered to accommodate two forms of mitochondrial donation. These techniques differ in their potential ethical implications so understanding the difference is important. The aim is that through these techniques, generations of children will be saved from mitochondrial disease. They are called maternal spindle transfer (MST) and pronuclear transfer (PNT).
The pre-requisite to any MRT therapy conducted is that the woman must have known mitochondrial defect with good chance of having a baby of high mitochondrial mutation. The defect caused should be directly from the mitochondrial DNA which, specifically excludes nDNA responsible for mitochondria. This defective mitochondrial DNA is also known to be severe. In all cases, the intended mother will have defective mitochondria in her eggs. The mitochondrial donor will be an egg donor whose egg contains healthy mitochondria. Also, for the sake of most optimal results, it will be helpful if the donor is young and healthy as well.
Maternal Spindle Transfer
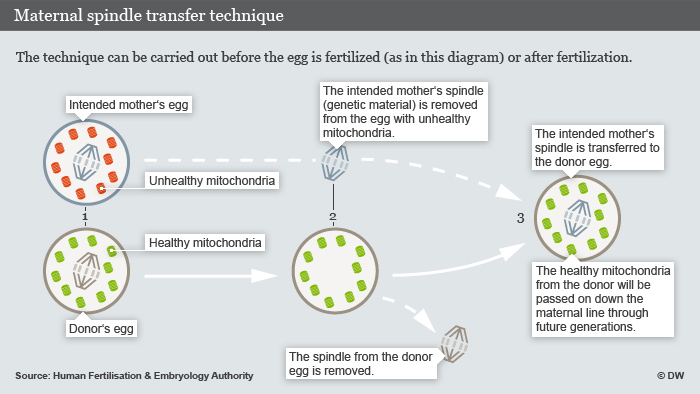
Figure 1: Maternal spindle transfer procedure
In maternal spindle transfer; as shown in figure 1, the exchange of genetic material takes place before fertilisation. The first step is, the nuclear DNA from the intended mother’s oocyte is removed. This leaves behind an enucleated egg cell filled with abnormal mitochondria. At the same time, the nDNA is removed from the donor egg. This leaves behind an enucleated egg with healthy mitochondria. In the second step, the intended mother’s nDNA is inserted into enucleated donor egg. The nDNA at the oocyte stage is in the spindle form, hence the name ‘maternal spindle transfer’. This new egg, now has intended mother’s nDNA surrounded by healthy mitochondria is ready for in vitro fertilisation with sperm. Then the regular procedures for IVF will apply. The end result being a healthy offspring of intended parents.
The potential limitation with MST is that when the spindle is removed, some of the defective mitochondria in the surrounding ooplasm may be slurped up. This can potentially contaminate the new hybrid oocyte. Nonetheless, this is likely to be a miniscule amount. Screening of the new egg through PGD can assure only healthy eggs are used for IVF.
Research done previously on monkeys (Tachibana et al., 2012) has been promising. Nonetheless, more study needs to be done to ensure safe and reliable outcomes.
Pronuclear Transfer
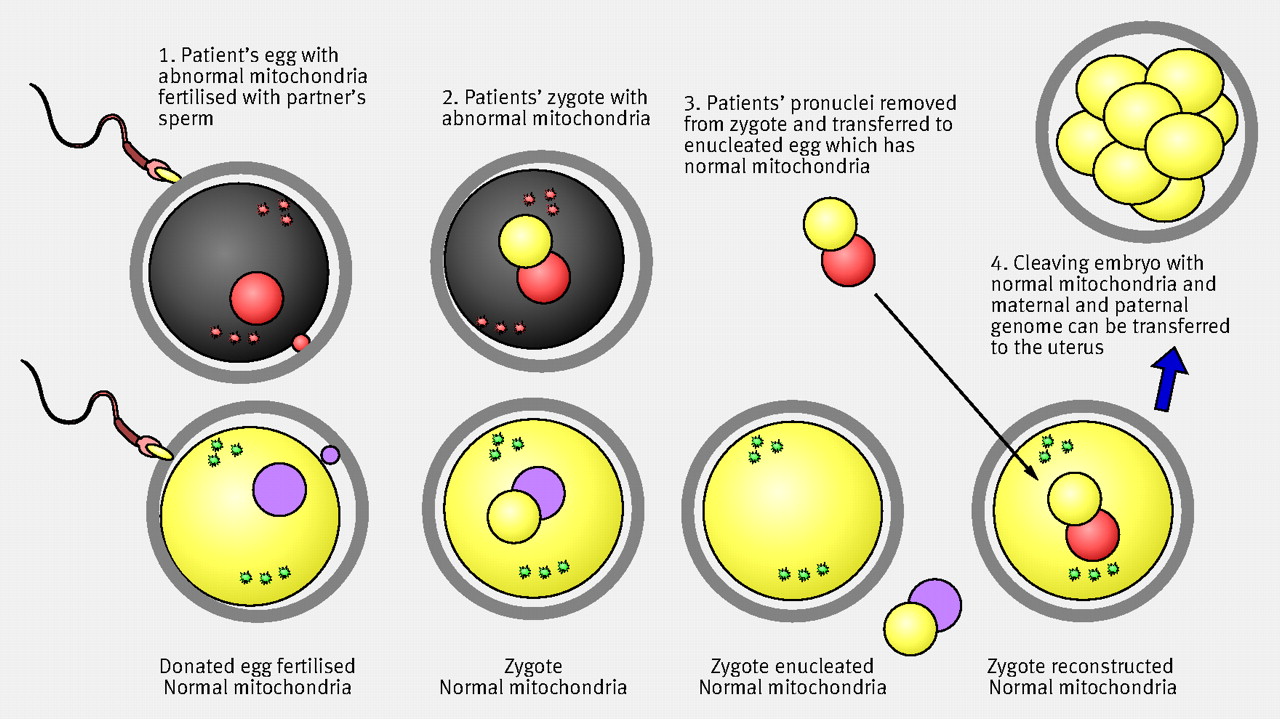
Figure 2: Pronuclear transfer procedure. Source Bredenoord and Braude (2010)
The second technique; as shown in figure 2, is called pro-nuclear transfer (PNT). In this technique, the exchange of genetic material takes place after fertilisation. The first step is that the intended parental eggs are fertilised forming a zygote with unhealthy mtDNA but intended parental DNA. At the same time, the intended father’s sperm is fertilised with the mitochondrial egg donor forming a zygote with healthy mtDNA but nDNA recombination of intended father and donor. In the second step, the pronuclei is removed from both zygotes. Thirdly, the intended parental pronuclei is placed into the zygote with healthy mtDNA. This zygote is let to divide and grow to day 5 and then placed in intended mother’s womb for implantation. In total two zygotes are formed, one is discarded and destroyed whilst the other is used for therapy.
PNT in mice (Sato et al., 2005) proved successful. The offspring were free of parental disease. Lindsey Craven and her team (2010) demonstrated that zygotes from PNT can progress onto blastocyst stage in vitro.
Differences between MST and PNT
1) MST occurs before fertilisation stage whilst PNT is a post-fertilisation technique.
2) In MST, the defective mitochondrial enucleated oocyte is discarded whilst in PNT, the defective mitochondrial enucleated zygote is discarded.
In 1990, Jacques Cohen (Cohen et al., 1997) undertook a technique similar to MRT in the US. It is useful to appreciate this study. This study involved the use of ‘ooplasmic transfer’. This is where a small amount of ooplasm from a healthy egg donor was extracted and injected into oocyte affected with defected mitochondria. The aim was to rejuvenate the eggs for better health. The end results were not well published. However, out of the 28 attempts in 25 women with fertility issues, there were 12 successful pregnancies. Although scientifically a decent result, medically it meant more than half of the women suffered. Only one known case out of these 12 was followed up properly (Karen Weintraub, 2013). This was the case of the teenager Alana Saarinen. She is well and healthy and her mother is very pleased with the results (Moses Gold, 2013).
Despite one known optimal outcome for ooplasmic transfer, the FDA (food and drug administration) put a halt to further research (Casper et al., 2002). This is because medically, ooplasmic transfer did not yield good enough results. The lessons learnt from ooplasmic transfer are the importance of keeping all experimental data, to keep a regular progress check on the babies conceived for as long as possible and if repercussions occur, the law can stop further testing.
New law approved by the UK parliament
The new law approved by the UK parliament was made on 4th March 2015 and will come into effect on 29th October 2015. The latest additions in Human Fertilisation and Embryology (Mitochondrial Donation) Regulations 2015 are relating to the two proposed techniques MST and PNT.
The Human Fertilisation and Embryology (Mitochondrial Donation) Regulations of 2015 has 3 parts. The first part is pertaining to clarification of terms used in the law, and the extent of their meaning. These include defining the ‘polar body nuclear DNA’ as all nDNA in a polar body or the term ‘removal’ as meaning destroyed. It is important to understand the terms so no doubt will remain about the procedure legalised.
The second part of the laws on Mitochondrial Donation is about ‘permitted eggs and permitted embryos’. These are eggs and embryos created specifically for MST and PNT respectively. These cannot be used for any other purpose than that intended for the techniques. No other alterations are allowed for the eggs and embryos in these two processes. The methods of the two techniques; MST and PNT, are clearly laid out in this part. This part ends with a note on using eggs and embryos in this process and circumstance just for the purposes of mitochondrial donation. These eggs and embryos are not to be considered the same as ‘permitted eggs and embryos’ used in other fertilisation processes. They are especially created for MRT and can only be used for this purpose alone.
Also in the second part of the law, there are pre-requisites given for the type of person applicable for mitochondrial donation. This has to be a woman whose eggs have mitochondrial abnormalities. These abnormalities need to be significant enough that they could potentially cause severe mitochondrial disease.
The third part of the law is relating to matters surrounding mitochondrial donation once it has taken place. This specifies that specific but non-identifiable data about the donor will be given to any children born from mitochondrial donation. The donors will have access to similarlylimited data if they wish to acquire it. It is interesting to note that the law specifies there is no relation between the mitochondrial donor and any children born from her egg, and hence marriage or physical intimacy is potentially legally possible. As such, children from the same donor are not notified. The mitochondrial donor is not allowed to be a parent to the child. No relation is formed between child and mitochondrial donor. Thus, legally no familial connection between the children is formed.
In part three of the law on mitochondrial donation, it states that once the procedure has taken place whereby the nuclear DNA of the intended mother is placed into the enucleated egg or embryo of mitochondrial DNA, the donor cannot take back her consent. As such, the egg/embryo formed through mitochondrial donation is also not considered the egg/embryo of the donor. The donor is simply a mitochondrial donor. This point has been re-iterated because legally, the mitochondrial donor cannot be considered a parent on the mitochondrial contribution merit alone.
The law is thus very careful to ensure the correct use of eggs, embryos and sperm for the specific purposes of MRT. These are not to be exploited for any other reason. The law is also very precise on the techniques used. This will ensure again that any risks of fatalities or abnormal births can be reduced as well as clarifying techniques. Following which, the law is now put into place to describe mitochondrial donors as egg donors without any parental rights. Egg donors are being used effectively as tissue donors. This will minimise ethical concerns of parenthood.
An over-view of the Islamic Law will help to contextualise the ethical questions raised. A combination of the UK law mixed with Islamic Law will give the ethics of MRT a richer medium of discussion in its applicability in the Muslim world.
The Shari’a or the Islamic law in general is quite strict and obvious. However, in some cases, there is room for interpretation of the Qur’an and the teachings of the Prophet (pbuh). This often means in certain technical issues Islamic law can differ from one country to the next. Therefore, it is important to understand the Shari’a of human fertilisation first and then to apply it for MRT.
The first criterion for a couple seeking fertility treatment is that they should be married. The second is that sperm donation is not allowed. This is because it breaks the sanctity of wedlock at a cellular level. As such, egg donations are not either (Aida I Al Aqeel, 2007). However, if the egg donor is also the co-wife of the woman needing the egg, then this is acceptable (Albar, 1999). According to the Islamic World League discussion in Saudi Arabia in 1998, genetic engineering to prevent disease or to treat without causing any further damage is possible.
Ethical questions arising due to MRT
The ethical questions raised by mitochondrial donation are relating to Beauchamp and Childress’ principle of ‘beneficence’ (Beauchamp and Childress, 2001). The benefit of having children without the debilitating condition caused by mitochondrial defect much out-weighs the harm of MRT’s unknown trial-like quality. There is an element of taking preventative measurements before the disease occurs, right at the point of conception. This needs to be done though in accordance with the principle that those involved are protected from physical, emotional and all other harm. This is because in trying to do good for those with severe mitochondrial defect, there may be negative outcomes. In this section I explore the various ethical issues surrounding mitochondrial defect.
Identity
It is a common query that since a door egg has been used, whom exactly does the child born belong to? The nuclear DNA is of the intended parents but the mitochondrial DNA belongs to someone entirely different. Can we look at these as two separate entities? The nDNA defines almost all of the offspring and the mtDNA only makes up a minute yet vital part. Sally Davies, the UK’s chief medical officer likened the defected mitochondria to a faulty car battery (Nick Collins, 2013). The car cannot work if the battery is down but it does not define everything else in it.
Considering there is a minute part of another woman’s egg in the new mtDNA donation offspring, would this donor have any part in considering the child her own and vice-versa? The UK law has stipulated that no relation is formed through this form of egg donation for mitochondria replacement therapy. A mitochondrial donor can come forward without repercussion of parenthood later on. Also, this would make more women open to the idea of mitochondrial donation.
In any case, fertilisation occurs between nuclear DNA of sperm and egg cell only. All else in the cytoplasm of the gamete cells does not undergo the transformation process. Hence, the donor egg cell DNA is not involved in the fertilisation process. The mitochondria are simply replicated on to the daughter cells. The donor egg woman cannot be considered a ‘third’ parent. To say MRT is forming ‘three-parent babies’ is inaccurate.
If mitochondrial donation took place under the Islamic context, would the mitochondrial donor be considered a ‘mahram’ to the child? A mahram is kin with whom marriage or sexual relations are prohibited. Only the woman who gestationally bears and gives birth to the child is considered the mother, as the Quran says ‘none are their mothers except those who gave birth’ (chapter 58, verse 2). There is no exception given to surrogates and hence Islamically surrogacy is not allowed. Only 0.02% of the child created belongs to a woman other than the gestational mother.
Dr Muhammad Ali Albar, director of the Medical Ethics Centre (Jeddah) critiqued that babies breastfed more than five full times by a woman are considered her mahram. This brings the question whether those who have mitochondrial DNA from the donor are mahrams too? This is something Professor Ebrahim- one of the most notable Islamic Bioethicists from University of KwaZulu-Natal, South Africa, also pointed out. The bond formed by a milk mother is that nutrition is passed on from woman to baby. However, in the case of mitochondrial donation, vehicles of energy consumption are being passed on. In the Muslim milk banks, due to the quantity of milk donated, the process is anonymised (Ghaly, 2012). This minimises milk-bonds.
Germline modification
MRT does cause a direct change in the germline of mitochondrial DNA. Children born via MRT form of IVF will have nuclear DNA from their parents and mtDNA from a donor. All girls born from this line will thus always carry mtDNA from the mitochondrial egg donor. The boys will not cause a germline modification as mitochondrial defect is only maternally passed on.
Mitochondrial DNA is the same for siblings and even cousins in a family. It is not unique like nDNA. The lack of individual specificity makes mtDNA replacement a less sensitive issue.
Girls born through MRT will carry on their progeny free of mitochondrial disease. This is a positive change. However, it has not been proven yet as MRT is still in its infancy. Hence, MRT is proposed initially for producing boys. This will limit germline alterations until the technique assures safe results (Bredenoord et al., 2010), whence it will be used for girls.
MRT is experimental
MRT is in its primitive stages. The HFEA drafted regulations to moderate the therapy as best they can. This would safeguard the families involved as well the physicians in their care. MRT is experimental and will most likely be for a few generations to come. Any adverse effects caused might not be curable. Hence, this technique is to be taken with caution and care.
As with all experimental new techniques, psychological examinations of potential candidates are important. The couple needs to be strong enough to deal with any negative results. It is assumed that any couple applying for MRT would have suffered a lot that they are referred for this technique. Hence, they are likely to be prepared. Both the wife and husband will need to be prepped and counselled. MRT is not simply a wife’s decision but a choice made by the couple itself in order to support one another. As such, a consent needs to be sought,
MRT does need to be moderated strictly. The regulations were thus very precise in the law on mitochondrial donation. As well as this, there should be key quality indicators at each step of the process to ensure safe optimal results. It is vital to have regular check-ups and follow-ups on the couple and baby born. This should be a life-long process so all results can be monitored and maintained for review. This was a huge problem of the ooplasmic transfer technique. There were next to no follow-ups and hence little can be gained from that study.
There are three possible outcomes of MRT. One that the couple conceive a healthy baby, second that the baby is miscarried and third that the baby born has some kind of disease of an unknown source (Baylis, 2013). In the case of the first scenario, only regular follow-ups will be required. In the second scenario, the couple will need bereavement counselling. In the third scenario, the couple need to be given counselling that the most qualified team did the best for them.
At some point, experts in the field of MRT will need to get together and assess the suitability of this procedure. Only if the success rate is high enough then more patients can be taken on.
There is a huge worry that MRT would cause a ‘slippery slope’ into the creation of designer babies. Possibly? However, the fact remains that the nDNA remains untouched and whole (Bredenoord et al., 2008). It is not being tampered with in any way. Nor any suggestion has been made to the effect. The only part being utilised is an egg donor’s enucleated egg.
Donor
The donor plays a vital role in the ethical debate. Firstly, is the donor considered an egg donor or tissue donor? This difference needs to be understood so her role is possibly better understood. Islamically speaking this difference will dictate the rights of the donor.
In the UK, an egg donor will simply need to consent to egg donations but with the knowledge that they will be used for mitochondrial donation. This will ease her mind that no nDNA is inherited. It may mean more donors will come forward for MRT. The law will grant the egg donor anonymity and freedom from all maternal obligations. Under all circumstances, the egg donor will need to be given full information about her input, the procedure of egg donation and all relevant knowledge.
With regards to the Islamic Ethical implications, it is important to note that the donor egg DNA is not being used in the fertilisation process in MST. Hence, the donated egg should be considered the same as a tissue donor. This is the opinion of Professor Ebrahim.
Dr Tariq Ramadan- the director of CILE, commented that the main ethical issue in MRT is raised by the egg donor. A sperm donor would not be allowed under any circumstance. Professor Ebrahim agreed with this. A child ought to be born under the premise of marriage. This issue is based around sanctity of marriage, and family life. A man can marry up to four women and woman cannot. A man can only marry more than one woman if he can treat his wives equally, in terms of money, living and time. Therefore, egg donation can be considered but sperm donations are not allowed. If the donor egg is fertilised by the man’s sperm, it is unlawful and considered zinaa. On the other hand, if one of the wives of the man donated her egg for another wife, it would be acceptable Islamiclly. This is one solution to the egg donor problem.
The co-wife’s egg donation would be a suitable solution for those under-going PNT. In pronuclear transfer, the intended mother’s egg and the donor egg are first both fertilised by the intended father’s sperm. Then the donor egg pronuclei are discarded. The intended mother’s egg pronuclei are placed into the donor enucleated egg. Due to the fertilisation of both maternal and donor eggs, this is a procedure that would Islamically only be acceptable with the use of the man’s other wife’s egg. The other wife too has the option of accepting or declining egg donation. Her willing consent is needed, and she should not be coerced in any way.
The procedure of MST allows for the maternal spindle of intended mother and donor to be removed prior to fertilisation. The maternal spindle of the intended mother is placed in the enucleated donor egg. Then fertilisation takes place. This is a technique that could make use of an egg donor, whereby the donor is considered the same as a tissue donor, as Professor Ebrahim found acceptable. Thus, it can be acceptable to use an egg donor in the case of MST according to both Professor Ebrahim and Dr Tariq Ramadan. However, in the case of PNT, as the donor egg being fertilised, the issue of marriage is raised.
In the case of MST, the egg donor can be treated as a tissue donor whereby her details can remain anonymous. On the other hand, the PNT egg donor Islamically speaking will need to be known as the implications for this are vastly different.
Society
It would greatly help the cause of MRT if wider knowledge was spread about the technique. This would alleviate the notion of ‘three-parent babies’ and hence open people’s minds a bit more to the technique. It is vital to ensure people understand the difference in mitochondrial DNA versus nuclear DNA. It is important to impart that MRT is causing a fundamental change in the new egg without tampering with the core of the egg, the nuclear DNA itself.
Islamically speaking, there is a lot of heated debate. It stems from the combination of donor eggs being fertilised by sperm. This is an unprecedented occurrence as Islamic law is very strict on this. More awareness needs to be made that MRT in the two different forms can potentially be Islamically agreeable given certain circumstances. The techniques MST and PNT are different technically as well as ethically.
MRT is in its early stages still. Hence, prominent Islamic Bioethicists such as Muhammad Ali Albar would like to see successful results from MRT before passing a bill to allow for this technique to take place in the Muslim world.
Eligibility
MRT should be governed strictly at the beginning. It should be specifically for cases where there is known mitochondrial defect in the woman caused by DNA mutation in the mitochondria themselves. This couple should have tried to have normal pregnancies. After perhaps two miscarriages they should be allowed to have MRT. The couple should also be psychologically stable to handle the consequences of this technique and its follow-ups. It would be useful if the woman was otherwise fit and healthy and of good child-bearing age to carry the pregnancy through to term.
Please continue reading the second part of this article here
Part 2 of 2

Opinions of scholars and intellectuals I have interviewed
While doing this work on MRT, opinions from various scholars and intellectuals in the Islamic and scientific field were sought. The main question posed was if MRT could be considered an ethically sound procedure.
Dr Tariq Ramadan and Professor Ebrahim feel MST can be allowed, given that fertilisation of sperm and donor egg is not taking place. Therefore the egg donor can be treated like a tissue donor. Both Islamic Bioethicists also feel that PNT can have a place in the Muslim World given the man is married to both the intended mother and the consenting egg donor.
It is interesting to note, during surveys done in the UK on the acceptability of MRT, some people were concerned about PNT. To them, it felt like discarding the donor egg pronuclei was the same as destroying an embryo.
Dr Muhammad Ali Albar and Dr Babar Haroon, an intensive care internist from Dalhousie University, have said that removing a harm that is of the intensity caused by mitochondrial defect should be considered praiseworthy. They both suggested that MRT seems acceptable. Dr Muhammad Ali Albar stressed however that this was his own opinion and would need to go through the Islamic Council of Bioethics. Currently, Saudi Arabia permits egg/sperm donations ‘between spouses, without intervention of a third party in the reproduction process and it must be done when there is a valid marriage contract in place and they are both alive.’
Dr Abdel Majid Katme has been working with pro-life lobbyists and conservative Christian groups in the UK comdemning MRT. This is based on his reasoning that MRT is forming babies with three parents. Dr Abdallah Mangoud and Dr Maged Gharib have suggested that MRT should not be allowed because of the genetic manipulation caused in MRT. Dr Amin Kashmeery (head of Biomedical Ethics section at King Saud Abdulaziz University in Saudi Arabia) has said that further discussion needs to take place, with more research especially after studies have taken place on the results of the procedure of MRT itself.
Conclusion
Mitochondrial Replacement Therapy is a novel technique in the field of IVF. It is firstly an experimental technique. There has been some success relating to procedures involved in MRT, however, on the whole, this will be the first of its kind. MRT is for women who are unable to conceive properly because mutated mitochondria in their eggs are too high to support life. Therefore, they suffer miscarriage after another or bear babies that die young.
Mitochondrial disease is maternally passed on. There are two techniques proposed for MRT that are known as maternal spindle transfer and pro-nuclear transfer (PNT). In both techniques, the donated egg has healthy mitochondria. The nucleus of the donated egg is removed and discarded. In MST, the nucleus which is in the form of a spindle, is removed from the donated egg. The maternal spindle from the intended mother’s egg is removed and placed in the enucleated donor egg. This is then fertilised by the father’s sperm. In pronuclear transfer, the intended mother’s egg and the donor egg are bother fertilised by the intended father’s sperm. The pronuclei in the donor egg is removed and discarded, whilst the pronuclei in the intended mother’s egg is removed and placed in the enucleated donor egg. MST takes place before fertilisation and PNT is a post-fertilisation technique.
There has been some success found until the blastocyst stage. This is the stage just before implantation. Scientists have found that an egg formed using a mitochondrial donor egg can successfully fertilise and divide.
The tricky thing relating to MRT is that it involves DNA of three people. The nuclear DNA of both intended parents and the mitochondrial DNA of a donor. The UK Law coming into action on 29th October 2015 has concluded that this donor material is not considered the same as an egg donor for other fertilisation treatments. As such, the egg donor will have no repercussions of being a parent to the baby born. Similarly, some Islamic Bioethicists have concluded the same for one of the techniques involved in MRT. In MST, the egg donor is to be treated the same as a tissue donor. According to the UK, specific data relating to the donor will not be revealed.
Egg donor-ship on the whole causes uncomfortability for Islamic rationale. The sanctity of marriage prevents access to egg donors. If scientific explanation can over-come this, then it could be allowed.
The fact that mitochondrial donation is in its early experimental stages, and results are unknown, means people are weary of giving their opinion. It is important to see a technique works before it can be given ethical approval. If a technique intended for bringing therapy actually causes harm, of an unknown origin too, then no one can ever approve of it. The rest of the world will be watching the UK, to see if they can make MRT a reasonable solution for those suffering mitochondrial disease.
If MRT is not successful, the ethical debate can be closed. If MRT is found to be successful, then it is important to understand the scientific implication on ethics for this procedure.
References and Bibliography
Aida I Al Aqeel, 2007. Genetic Counseling in the Muslims World: The Challenges. Presented at the 2nd Pan Arab Human Genetics Conference, Centre for Arab Genomics Studies, UAE.
Albar, M.A., 1999. Counselling about genetic disease: an Islamic perspective. East. Mediterr. Health J. Rev. Santé Méditerranée Orient. Al-Majallah Al-Ṣiḥḥīyah Li-Sharq Al-Mutawassiṭ 5, 1129–1133.
Baylis, F., 2013. The ethics of creating children with three genetic parents. Reprod. Biomed. Online 26, 531–534. doi:10.1016/j.rbmo.2013.03.006
Beauchamp, T.L., Childress, J.F., 2001. Principles of Biomedical Ethics, 5th ed. ed. Oxford University Press, 198 Madison Avenue, New York, New York.
Bredenoord, A.L., Braude, P., 2010. Ethics of mitochondrial gene replacement: from bench to bedside. BMJ 341, c6021–c6021. doi:10.1136/bmj.c6021
Bredenoord, A.L., Dondorp, W., Pennings, G., Wert, G.D., 2010. Avoiding transgenerational risks of mitochondrial DNA disorders: a morally acceptable reason for sex selection? Hum. Reprod. 25, 1354–1360. doi:10.1093/humrep/deq077
Bredenoord, A.L., Pennings, G., Wert, G. de, 2008. Ooplasmic and nuclear transfer to prevent mitochondrial DNA disorders: conceptual and normative issues. Hum. Reprod. Update 14, 669–678. doi:10.1093/humupd/dmn035
Brown, D.T., Herbert, M., Lamb, V.K., Chinnery, P.F., Taylor, R.W., Lightowlers, R.N., Craven, L., Cree, L., Gardner, J.L., Turnbull, D.M., 2006. Transmission of mitochondrial DNA disorders: possibilities for the future. Lancet Lond. Engl. 368, 87–89. doi:10.1016/S0140-6736(06)68972-1
Bruce H. Cohen, 2000. Mitochondrial Cytopathies: A primer.
Casper, R., Lazendorf, S., O’Reilly, M., Cohen, J., Patterson, A., Rose, S.M., 2002. Biological Response Modifiers Advisory Committee Open Session. www.fda.gov, Hilton Hotel Gaithersburg, Maryland.
Cohen, J., Scott, R., Schimmel, T., Levron, J., Willadsen, S., 1997. Birth of infant after transfer of anucleate donor oocyte cytoplasm into recipient eggs. Lancet 350, 186–187. doi:10.1016/S0140-6736(05)62353-7
Craven, L., Tuppen, H.A., Greggains, G.D., Harbottle, S.J., Murphy, J.L., Cree, L.M., Murdoch, A.P., Chinnery, P.F., Taylor, R.W., Lightowlers, R.N., Herbert, M., Turnbull, D.M., 2010. Pronuclear transfer in human embryos to prevent transmission of mitochondrial DNA disease. Nature 465, 82–85. doi:10.1038/nature08958
Elliott, H.R., Samuels, D.C., Eden, J.A., Relton, C.L., Chinnery, P.F., 2008. Pathogenic mitochondrial DNA mutations are common in the general population. Am. J. Hum. Genet. 83, 254–260. doi:10.1016/j.ajhg.2008.07.004
Foetus with three parents created, 2003. . BBC.
Ghaly, M., 2012. Milk Banks Through the Lens of Muslim Scholars: One Text in Two Contexts. Bioethics 26, 117–127. doi:10.1111/j.1467-8519.2010.01844.x
Gray, M.W., Burger, G., Lang, B.F., 2001. The origin and early evolution of mitochondria. Genome Biol. 2, 1018.1–1018.5.
Human Fertilisation and Embryology (Mitochondrial Donation) Regulations 2015, 2015.
Karen Weintraub, 2013. Three Biological Parents and a Baby. Well NY Times.
Mitochondrial DNA [WWW Document], 2013. . Genet. Home Ref. URL http://ghr.nlm.nih.gov/mitochondrial-dna (accessed 2.8.14).
Moses Gold, 2013. Michigan Girl, 13, Ends Up With Three Biological Parents | Religion [WWW Document]. Its News Altern. News UFO Sci. True News Prophecy News People Powered News. URL http://beforeitsnews.com/religion/2013/12/michigan-girl-13-ends-up-with-three-biological-parents-2461010.html (accessed 1.28.14).
Nick Collins, 2013. Babies with three parents: Britain gives green light to radical IVF plan - Independent.ie [WWW Document]. URL http://www.independent.ie/life/family/mothers-babies/babies-with-three-parents-britain-gives-green-light-to-radical-ivf-plan-29379540.html (accessed 10.28.15).
Possible Symtoms, 1996.
Robin Clarke, Remco van der Stoep, 2013. Medical Frontiers: Debating mitochondria replacement. Office for Public Management.
Rodney Shackelford, 2011. The Mitochondrial Theory of Aging. H Mag.
Sato, A., Kono, T., Nakada, K., Ishikawa, K., Inoue, S.-I., Yonekawa, H., Hayashi, J.-I., 2005. Gene therapy for progeny of mito-mice carrying pathogenic mtDNA by nuclear transplantation. Proc. Natl. Acad. Sci. U. S. A. 102, 16765–16770. doi:10.1073/pnas.0506197102
Schaefer, A.M., Taylor, R.W., Turnbull, D.M., Chinnery, P.F., 2004. The epidemiology of mitochondrial disorders--past, present and future. Biochim. Biophys. Acta 1659, 115–120. doi:10.1016/j.bbabio.2004.09.005
Tachibana, M., Amato, P., Sparman, M., Woodward, J., Sanchis, D.M., Ma, H., Gutierrez, N.M., Tippner-Hedges, R., Kang, E., Lee, H.-S., Ramsey, C., Masterson, K., Battaglia, D., Lee, D., Wu, D., Jensen, J., Patton, P., Gokhale, S., Stouffer, R., Mitalipov, S., 2012. Towards germline gene therapy of inherited mitochondrial diseases. Nature 493, 627–631. doi:10.1038/nature11647
Taylor, R.W., Turnbull, D.M., 2005. Mitochondrial DNA mutations in human disease. Nat. Rev. Genet. 6, 389–402. doi:10.1038/nrg1606
Types of Mitochondrial Disease - The United Mitochondrial Disease Foundation [WWW Document], n.d. URL http://www.umdf.org/site/pp.aspx?c=8qKOJ0MvF7LUG&b=7934629 (accessed 10.28.15).
UK Legislation, 2008. Human Fertilisation and Embryology Act 2008 [WWW Document]. legislation.gov.uk. URL http://www.legislation.gov.uk/ukpga/2008/22/section/26 (accessed 12.27.13).
UK Parliament, 2015. Commons Debate.
Wai, T., Teoli, D., Shoubridge, E.A., 2008. The mitochondrial DNA genetic bottleneck results from replication of a subpopulation of genomes. Nat. Genet. 40, 1484–1488. doi:10.1038/ng.258
www.mitomap.org, 2013. Pathological Mutations in tRNA.
Appendix 2: Opinions of scholars and physicians
Dr. Mohammad Ali Albar FRCP, Director of Medical Ethics Centre IMC, Jeddah, Saudi Arabia.
Permissible
-
Genetic material in nucleus
-
Maternal mitochondria in cytoplasm
-
Mitochondrial genes small in number
-
Cytoplasmic material of donated egg has an infinitesimal small number of genes
-
Mitochondrial genes can cause serious congenital disease
-
In-vitro fertilisation can avoid maternal mitochondria by using enucleated egg from donor
-
Resembles cloning with a difference. 99% genes from intended parents.
-
In Shari’ah avoiding harm takes precedence, in this case, to avoid a fatal disease
-
Genetic material is from intended parents
-
From understanding of Islamic Ethos and Fundamentals of Islamic jurisprudence, MRT is permissible
-
Personal opinion
Suggogacy discussion in Makkah at the Muslim World League in 1984
- This subject needs extensive study by jurisprudential academics specialised in this branch of Medicine
- The new research emphasizes the effect of environmental factors on genes and their function
- Hence, Al Razi and Ibn Sina recommend choosing a breastfeeding mother carefully because of its impact on the infant’s morals and behaviour
- Maybe this is why the breastfeeding mother is considered a second mother (despite no actual blood relation)In cosmetic surgery, to remove a harm in order to restore normality is commendable
- MRT can be included in this category with some reservations
Brought to light by Professor Abdullah Al Sayan
- Not allowed unless husband has two wives and co-wife accepts to carry
- This fatwa withdrawn in 1985
- Qu’ran, ‘None are their mothers except those who gave birth’ (Chapter 58, Verse 2)
- Sperm donation is not allowed
- Ovum uterus or somatic cell donation not allowed
- Ali Khamenei permitted anonymous donation of sperm and egg in infertility cases
- A lot of Shi’a clerics do not agree with Khameni
- Fuqaha agree gamete donation is limited between spouses only with valid marriage contract and both are living
- ‘Three-parent’ scenario occurs in those with Muslim background
- A child with a milk mother* effectively has three parents
Information on Advanced Medical Directives by Dr. Muhammad Ali Albar. Treatment choices are 5:
1. MUST in emergency cases and cases of infectious disease which have a cure
2. COMMENDABLE in all cases that have a cure
3. PERMISSIBLE in cases where medicating or not are even
4. DISFAVORED when risk of treatment out-weighs the benefits
5. IMPERMISSIBLE in talisman, magic and fortune-telling
Wine and pig are generally forbidden unless no alternatives and prescription by Muslim physician
Dr. Abdel Majid Katme MBBCH, DPM, Spokesperson: Islamic Medical Association/UK on Medical Ethics, Weekly TV presenter of an Islamic Health show, Muslim Coordinator to the Society for the Protection of Unborn Children (SPUC)
Impermissible
- Involved with pro-life organisations against legalisation of ‘3-parent’ childen
- Abnormal way of creating baby
- Qu’ran ‘no change to the way a baby is made/created’**
- Risky to take fatwa from Muftis without medical knowledge and qualifications
- Appeal to join cause against MRT
Mitochondria provides energy for cell function - Mitochondria has its own DNA/genes
- Mitochondrial defect comes from the maternal line (not paternal)
- Proposed idea to use healthy mitochondria from donor egg and ‘throw away the egg’
- Place healthy mitochondria into ‘woman who wants to have a child after emptying her egg cell from the diseased mitochondria’
- Then IVF with ‘new mixed egg’ with sperm of husband/partner
- Resultant child has ‘at least 3 parents, a father, a mother, and another mother who gave the genetic healthy mitochondria taken from her egg cell’
- Genes from three people, instead of the norm 2 (mother and father)
- This is changing sacred way of the creation of child
- Child will have confused identity
- Implications of this manipulation unknown
- Not normal way of life
- Genetically modified
- Acquisition of egg requires hormone injection to stimulate egg production- can be harmful
- Many Christian organisations against this unethical immoral proposal
Professor Amin Kashmeery, Professor of Physiology, Head of Biomedical Ethics at King Saud Bin Abdulaziz University for Health Sciences, Saudi Arabia
Unsure, undecided since he believes full evidence is not in yet
- Mitochondrial DNA is small in quantity
- Function of mitochondria is essential
- Hence, to what extent can it contribute to traits of personhood of off-spring
- Mitochondrial DNA mutation involves multiple organs
- These organs are vital and require a lot of energy
- Most notable is intellectual loss of function
- Mitochondrial DNA is rearranged via recombination and remains unchanged when passed from parent to offspring
- Helps to track ancestry down hundreds of generations
- Used in forensics
- Mitochondrial DNA helps assessment of genetic relationships between individuals therefore quantifying evolutionary relationship
- Mitochondrial DNA data helps biologists to form a relationship network among various sequences
- Ethical implications require more thought
-
Mitochondrial inheritance is through mother, ‘matrilineal inheritance’
-
Interaction between nuclear DNA with mitochondrial DNA can make this a ‘three-parent’ baby*** and therefore questionable
-
Makkah-based Fiqh Council of the Muslim World League did not allow use of second wife of the same man to be a surrogate
-
This is despite the second wife carrying sperm and ovum of another wife
-
This issue deserves debate
Dr. Abdallah Mangoud, Professor of Family Health and Medicine
Impermissible
- Based on Dr. Maged Gharib’s opinion
Dr. Maged Gharib MBBCh, MD, MRCP, FRCPath, Consultant Haematologist at St Helen’s and Knowsley Teaching Hospitals NHS Trust
Impermissible
- No long-term follow-ups yet
- Interaction between mitochondrial and nuclear DNA not fully understood yet
- ‘Three-parent baby’
- Avoiding fatal disease does not warrant this genetic manipulation
- To accept God’s will and avoid having children is the solution
- Supporting hadith: an epileptic lady asked messenger of Allah to be cured but he taught her patience was in her interest (without genetic manipulation)**
Dr. Babar Haroon, MD, FRCPC, Assisstant Professor, General Internal Medicine, Critical Care at Dalhousie University, Canada
Permissible
- The mitochondria is not involved in the fertilisation process
- The mitochondria are like the battery, and it is being replaced
- The nuclear genetic material remains that of the true parents
Professor Abul Fadl Mohsin Ebrahim, Professory Emeritus, School of Religion, Philosophy and Classics, University of KwaZulu-Natal, South Africa
Permissible given certain conditions
- Plausible novel technique however, issues from Shari’ah perspective
- The donor egg is cause of the problem
- Polygamous marriage is an easy way out of the donor egg problem, as donor would be another wife within wedlock
- However, polygamy is not the norm and there are thousands of women who suffer from this problem
- The status of egg donor cannot be considered like the milk mother to the child
- Access of egg by sperm can only be made through marriage according to Islamic Law
- The donor egg is the vehicle of human life and milk from another mother is only for sustenance
- The danger of the equation of egg donor being the same as milk mother, the donor’s children become mahram to the newborn
- Pronuclear transfer (PNT) will not be acceptable (outside marriage)
- Maternal Spindle Transfer (MST) is acceptable if proven effective and safe
- In MST, the DNA of the egg donor is removed and replaced with wife’s DNA prior to fertilisation. Fertilisation thus only takes place between husband and wife genetic material. The mitochondria is only replicated onto daughter cells
- The resulting baby will have DNA of both legally married husband and wife, and healthy mitochondria of donor only
- With this in mind, the egg donor would not be mother for the following reasons:
1) The hadith states, ‘al wiladu li al-firash’, the baby belongs to the one who gives birth to it
2) DNA of the donor has been removed from her egg, and only mitochondria is needed
3) The egg donor should not be paid for her services like the milk mother. No mahram bonds shall ensue between her or newborn or her children and newborn
- Selection of males is permissible since mitochondria will not be transferred onwards
- In females, the donor mitochondria will be transferred on to offspring and that makes the procedure questionable – sex selection needs further discussion
- PNT is permissible for a man with multiple wives between his lawful spouses
- PNT is not permissible for man with one wife
- For a non-polygamous couple, MST is a solution
- The egg donor must be anonymous and should be considered as a tissue donor.
- The egg donor must render her services gratis, because sale of tissue and organs is impermissible
- Once you are clear as a scientist that mitochondrial donor does not contribute to the actual nutrition of the baby, then the egg donor becomes a true tissue donor (unlike milk mother).
Dr. Tariq Ramadan, Professor of Contemporary Islamic Studies, Oxford University and Director of the Research Centre for Islamic Legislation and Ethics
Permissible given certain conditions
- Sperm donation is not allowed
- This can be considered on the basis that egg donors are being used
- PNT is allowed in polygamous marriages but not otherwise
- MST allowed in normal non-polygamous marriages
- Unsure about the status of the egg donor as tissue donor or milk mother
- Something of the egg donor has been given to the newborn
- The dilemma lies in, what could be given by whom and the nature of the ‘given’
*Milk mother is a woman who breastfeeds a baby until the age of 2 years. If a baby has suckled to full feed on 5 separate occasions or more, he or she can be considered her ‘son’. The bond formed is known as ‘milk-bond’.
Mahram relationship is one is not permissible for the other for marriage. This would be considered incest. Parents and their children are all mahram of one another
** ‘So direct your face toward the religion, inclining to truth. [Adhere to] the fitrah (natural way) of Allah upon which He has created [all] people. No change should be in the creation of Allah. That is the correct religion, but most of the people do not know’. Chapter 30, verse 30, Quran.
*** For the purpose of this work, only those disorders relating to the mitochondria through its own DNA are explored. Any disorders as a result of mitochondrial genes found in the nuclear DNA have not featured in this thesis.

















Comments
Comment Subject
Add new comment